So, what did we learn from the modern neuroscience that is relevant to the title of this post?
To me, the most striking information is the neuroplasticity of the brain, which means the brain is not a physiologically static organ. It has the capacity to change throughout life based on experience. What that means is environmental changes could alter behavior and cognition by modifying the connections between existing neurons and also through neurogenesis (birth of new neurons).
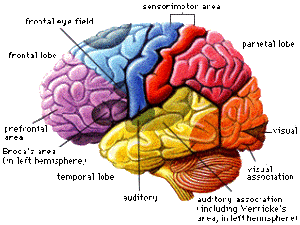
Exposure to trauma/traumatic events affects brain functions. Which part of the brain is affected the most depends on the developmental stage of the individual at the time of traumatic experience. If a person was socially-emotionally traumatized during the first year of life when the development of the brainstem is in full-swing, we might see problems in metabolism, hyperarousal or sensory perceptual problems rather than cortex or limbic based issues of guilt, identity, personal awareness, coping skills, etc. Although regions of brain that are immature and developing slowly are less likely to be severely affected by an early trauma, the affected lower brain structures often lead to inhibition of higher level brain function. Therefore the earlier, the worst.
The good news is that the damage of social-emotional trauma on brain is reversible thanks to neuroplasticity. This is of paramount importance for mental health professionals. The intervention strategies must be carefully tailored according to the brain region affected and the developmental level of the child at the time of trauma.
Brain regions respond to specific types of sensory input. Cognitive and insight-oriented interventions will have limited effect for a person traumatized very early in life. Non-verbal modalities such as sand play, art, movement therapies could provide alternatives to access low brain regions in order to modify connections in existing neurons.
At the end, psychotherapy of all kinds is a process of “corrective experience”. All we need to do is to access the specific brain region through specific types of sensory input. Sometimes it is “words”, some other times it is “kneaded, squeezed or cut-into-pieces of clay” that is worked in the presence of a quiet witness. As the neuroscientist Bruce Perry suggests, the bottom line is to use the neuro-developmentally appropriate therapeutic activities for the specific brain region affected.
Adopted from Play Therapy V. 5, Issue 4 p.18-20 December 2010